BY:
Kedar N Uprety, M.Comm.H
(UK)
Uma Basnet, MBA
Dil K Rimal, MPH
(With Cooperation of
Dr. N Rasalingam, President, Auckland Refugee Council)
Authors contact address:
3/8 Koromoko Street
New Lynn
AUCKLAND
Telephone: (09) 827 7571
E-mail address: mailbox@nznet.gen.nz
The research team would like
to thank those who helped during the process of this study. We are especially
grateful to the Auckland Refugee Council for giving us an opportunity to
analyze and understand the issues and concerns of refugees and asylum-seekers
in New Zealand. We would particularly like to express our gratitude
to Dr N Rasalingam who encouraged and supported us throughout the study
period. Our special thanks are also due to the organizer of National
Conference on Refugee and Asylum-Seeker Health for giving us an opportunity
to participate in the conference.
OTHER AGENCIES WORKING ON HEALTH ISSUES FOR REFUGEES AND ASYLUM-SEEKERS
METHODOLOGY
Data
Collection from the Records
Data
Collection Through the Conference
Ethical
Considerations
RESULT
Results
From the Records
Results
from the Conference
Figure 1
Attendance breakdown of Refugee Health Centre patients, 1992 - October
1998, by year
Figure 2
Patient attendance by health problems
Figure 3
Refugee status application and approval trends, by year
Figure 4
Refugee Health Centre patient flow, by year
Of the 185 member states of the United Nations (UN) only ten have established annual resettlement quotas above and beyond their acceptance of persons arriving spontaneously at their borders. New Zealand is one of these ten countries granting resettlement quota complying with guidelines set and overseen by the United Nations High Commissioner for Refugees (UNHCR). In a published document (Deloitte-Rose-Tomatsu, 1991) it is suggest that the estimated number of refugees in New Zealand (NZ) was 25,000 and that approximately more than 2,000 new refugees enter NZ every year. However, looking at the increasing number of both quota refugees and asylum-seekers to NZ in recent years suggested there are more than 35,000 refugees residing in NZ today.
Many asylum-seekers, (refugee status seekers) fleeing from situations of political unrest, terror, violence, and/or war, arrive in NZ in search of refugee status, but without legal documentation. In addition to the psychological impact of continuous exposure to intense, repeated, and often prolonged traumatic experiences such as war, rape, starvation, torture, loss of their families and their home country communities in the country of origin, asylum-seekers have usually left without having made any provisions for the future. Asylum-seekers both in detention and living in the community show evidence of profound depression, hopelessness and helplessness. In addition, low income, non-recognition of qualifications and poor quality housing, and lack of social support serve only to compound the day-to-day stress levels which have been identified as one of the more significant determinants of their ill health.
Unlike quota refugees, asylum-seekers do not undergo any effective medical screening until their application for refugee status is approved, a process which may take up to two years. It has been documented that the process of claiming refugee status in NZ is often stressful. Many asylum-seekers claiming refugee status remain in limbo for lengthy periods of time, facing uncertainty, interrogation by officials, the prospect of deportation and lack of access to health and social services. In their recent document, Silove, et al expressed concern that the interrogatory style of interviews by Immigration Service officials are likely to result in retraumatisation for asylum-seekers, especially given their previous experiences a majority of asylum-seekers have had with government officials in their countries of origin.
Being people in transition, asylum-seekers are particularly vulnerable when existing service mechanisms do not adequately address their problems. The existing health screening provisions available to refugees principally targets the needs of mandated or quota refugees, but not those of asylum-seekers. Inevitably, some asylum-seekers arrive with highly communicable diseased, eg, TB, HIV, STD, hepatitis, etc which is a major public health concern. Paradosically, existing health facilities and social services that asylum-seekers are entitled to are limited, yet the magnitude of health needs of asylum-seekers are greater and more serious than that of mandated refugees.
Since 1987, the staff at the Medical School of the University of Auckland have provided a voluntary service to asylum-seekers referred by their lawyers for medical examinations. To meet the needs of increasing numbers of asylum-seekers to NZ, the Auckland Refugee Council Incorporated (the Council) was established in 1987. In turn, this organization established the Refugee Health Centre (RHC) in 1992 to provide an acute medical service for both mandated refugees and asylum-seekers within the area served by the Council. Since its inception the Council has tried in earnest to help asylum-seekers fulfill their basic needs, often despite various intervention and distractions. While the Council's activities and resources remain limited, the steady increase in numbers of asylum-seekers relate proportionately to the ever increasing demands being placed on the Council's existing services currently provided by the Council include:
2. NZ AIDS Foundation (NZAF) - Burnett Centre: HIV testing. Counselling for those living with HIV and/or AIDS, their families, friends, partners. Counselling available to men who have sex with men, their male and/or female partners. HIV support services - buddies, home help, drivers, etc.
3. Oral Health Unit - Auckland Hospital: Emergency dental service. Relief of pain service. $40.00 for initial fee, further costs for additional visits.
4. Auckland Refugee Health Centre: Providing medical treatment and a specialist referral services for refugees. Free.
5. Auckland Sexual Health Clinic: Providing advice and information about sexual health, counselling, sexual health checks and treatment. A free and confidential service.
6. Community AIDS Resource Team (CART): HIV and AIDS support, counselling, information and referral service. Two social workers and a nurse provide personal support and assistance with: nursing care, medical management, access to housing, social welfare benefits and community services for all adult and children affected by HIV and AIDS in the Auckland region. Support service available for family and friends. Funding by Auckland hospital.
7. FGM clinic: A clinic providing obstetric/gynaecology care for women who have undergone Female Genital Mutilation. Free.
8. National Refugee Health Screening Centre: Providing health screening and health management for quota refugees at the Mangere Refugee Resettlement Centre (MRRC).
2. Maternal
Mental Health - A+: A mental health service for women who are
pergnant and up to one year postpartum, who are suffering from mental health
problems or severe psychological stress.
Although different organizations
and agencies are working to meet the health needs of refugees and asylum-seekers
the following facts reflect how patchy and inadequate existing services
are:
|
|
|
QUOTA REFUGEES | ASYLUM-SEEKERS |
| Accommodation for new arrivals
|
Provided at Mangere Resettlement Centre and housing is found for them on leaving | Should find on their own
|
| English language instruction
|
Receive language instruction at MRCC under auspices of AIT. Continue to be formally and routinely available when they move into the community | Not eligible for formal
language training during their first few months in NZ
|
| Introduction to NZ culture
|
An introductory programme to NZ culture is provided | No introductory programme to NZ culture is provided |
| Resettlement in NZ
|
|
|
| Unemployment benefit
|
Eligible for the usual unemployment
benefit including housing supplements and work permits
|
|
| Legal service
|
Do not need the assistance
of lawyer
|
Need legal advice, which is usually expensive, for the preparation and presentation of their cases |
| Access to health services
|
Have community services
card - thus can access health care
|
Usually takes long time to obtain a community services card, without which accessing a GP is difficult |
| Health screening
|
Receive comprehensive health
screening
|
Generally unavailable, although some organizations offer voluntary health screening, eg, Greenlane hospital, ARC |
1. Data Collection from the Records
The resarch team was asked by the ARC, under auspices of Council, to analyze patient records, as filed, dating from 1992 to October 1998. All such material was retrieved with the support of RHC staff. All records were manually tabulated prior to analysis. Charts and tables were produced by way of Microsoft Excel spreadsheet software. All mention of disease types contained in this report correspond directly with written diagnosis of the RHC medical coordinator. Some of the data were also collected from the records of New Zealand Immigration Service.
2. Data Collection Through the Conference
The research team also gained valuable, current information related to the purpose of this study from its participation at the "National Conference on Refugee and Asylum-Seeker Health" held on 17-18 November 1998.
All the material retrieved
from the RHC for analysis was treated in the strictest of confidence to
protect the privacy and identity of all individuals concerned. Details
of patients' names, addresses, etc have been entirely withheld from this
report.
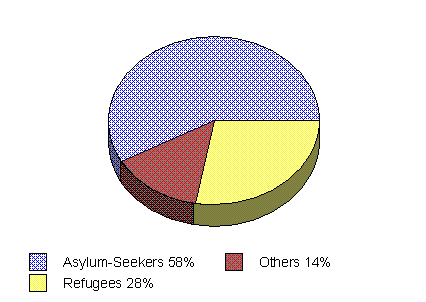
Figure 1: Attendance
breakdown of RHC patients, 1992 - October 1998 by status

Figure 1 indicates significantly
that the majority of referrals to RHC were asylum-seekers. This high
attendance characteristic for asylum-seekers could be due to RHC's services
being free-of-charge, since GP services for them are largely unaffordable.
Patients in the "Others" category of this chart identify as being either
permanent residents or as family reunification clients.
Figure 2: Patient
Attendance by Their Health Problems
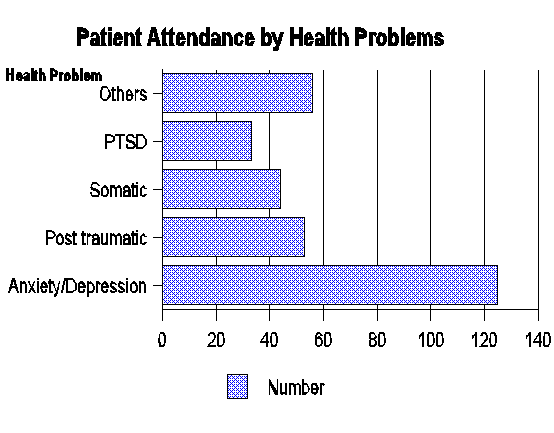
Key: PTSD =
Post Traumatic Stress Disorder
Figure 2 clearly indicates
that anxiety/depression is more than twice as prevalent as other health
complaints which are also of a serious nature. Communicable disease
complaints, which are grave concerns of public health, rate significantly
among "Others" category.
Figure 3: Refugee
Status Application and Approval Trends, by Year
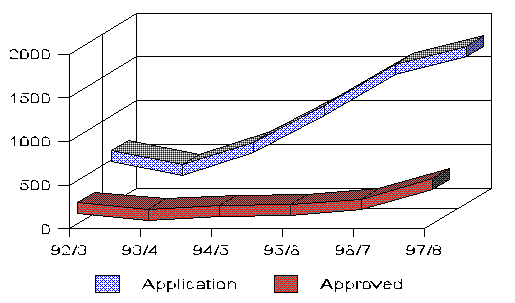
Source: New Zealand
Immigration Service
Figure 3 indicates how the
numbers of refugee status applications has steeply climbed in the period
1993/94 to June 1998 while, in the same period, the numbers of application
approvals has, with consistency, been disproportionately low. There
appears to be significance in the percentage of non-approved applications.
|
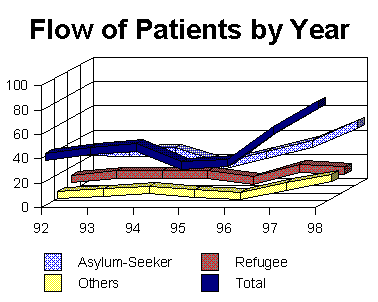
Source: Refugee Health Centre
Figure 4 indicates significantly
that while the throughput of patient referrals at RHC has doubled in the
past two years, the greatest increase in patient numbers has been with
those (patients) of asylum-seeker status.
|
2. Results from the Conference
As mentioned under methodology,
the research team had also participated in "the National Conference on
Refugees and Asylum-Seeker Health" to gain relevant background information
on refugee health-related issues. Mainly the issues raised and discussed
at the conference were about general problems/factors, which have negative
consequences on health. The following issues and problems were identified
at the conference:
The findings clearly show that there is a wider gap between demand and service provision for the asylum-seekers in Auckland. Therefore, there is a need for immediate action to address the multi-sectoral needs of the asylum-seekers.
The above findings show that the flow of asylum-seekers and refugees into NZ is increasing steadily every year, and available services offered for them are scattered and limited. The main problem exists in addressing the situation of asylum-seekers during the period of transition, being from their date of NZ arrival until when they obtain legal refugee status.
Looking at the increasing
inflow trend and multi-sectoral needs of asylum-seekers, there should be
a recognized Integrated Comprehensive Support Centre (ICSC) functioning
as a "one door shop" umbrella organization responsible for acceptable
and affordable health and social services being easily and reliably accessible
to asylum-seekers. Since many factors contribute to the ill-health
of asylum-seekers, the following ICSC programme (health and non-health)
should be designed in consultation with and with the participation of asylum-seekers
and refugees:
1. Deloitte-Ross-Tomatsu: An Investigation into the Special Health Care Needs for Refugees for the Auckland Area Health Board, 1991.
2. UNHCR, Protecting Refugees: Questions and Answers, 1996.
3. Ellis PK and Collings SCD (editor): Mental Health in New Zealand from Public Health Perspective; Public Health Report number, 1997.
4. Brochure/leaflet from the Auckland Refugee Council, 1998.
5. Wansbrough T, Public Health: Needs of Asylum-Seekers, 1998.
6. Refugee Health: Students Report (Unpublished).
7. Strategic Directions in Refugee Health Care, A Discussion Paper, NSW Health, 1997.
8. Refugee Services Directory Auckland, Auckland Refugees as Survivors Centre, 1998.
9. Briefing Paper to the Interdepartmental Committee on Refugees, 1998.
10. Silove D, McIntosh P, and Baker R, (1992): Retraumatisation of Asylum-Seekers (unpublished).
11. Statistics: New Zealand Immigration Service, 1998.
12. Hands out from the Speaker: National Conference on Refugee and Asylum-Seeker Health, November 1998.
13. UNHCR News Letter, Aug/Sept, 1998.
14. Refugees Magazine (UNHCR): No. 111, 112 Spring 1998.
15. Refugee Children, UNHCR, 1998.